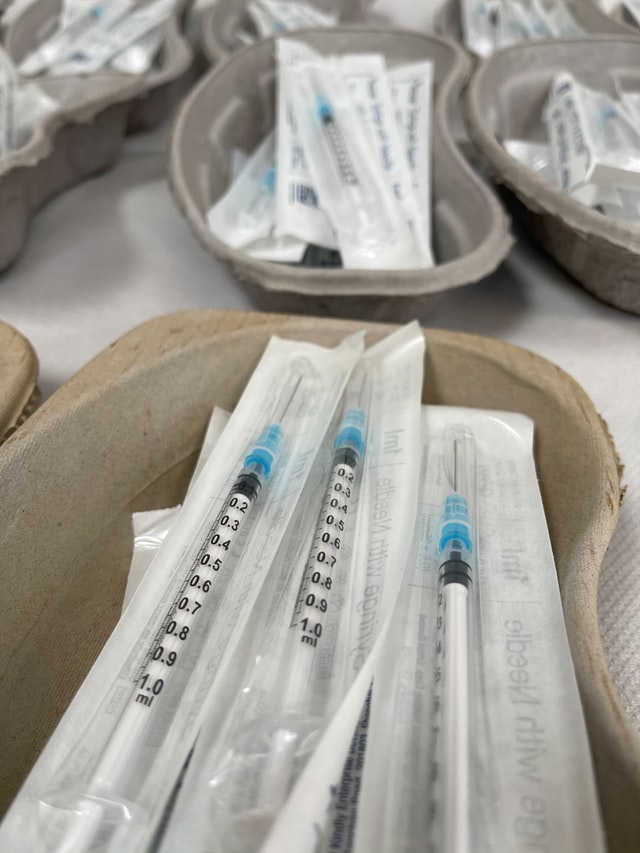
Feasibility study
A new report explores the feasibility, acceptability, and practical considerations of developing a peer-based needle exchange service, with additional hepatitis C awareness and testing capacity, in Hackney. The London Joint Working Group on Substance Use and Hepatitis C (LJWG) was funded by Hackney Council, as part of the ADDER Accelerator project, to undertake the exercise. ADDER (Addiction, Diversion, Disruption, Enforcement and Recovery) is the Government’s new flagship scheme to try to engage people with drug problems in contact with the criminal justice into treatment.
The need for more effective needle exchange services is clear. 43% of people who inject drugs reporting sharing needles or works in the four weeks prior to being surveyed and the overall level of hepatitis C transmission has changed little in recent years. In addition the number of serious bacterial infections amongst people who inject drugs has been steadily increasing since 2013. Peer educators from The Hepatitis C Trust facilitated the focus group interviews.
The report
The scoping report is based on three focus groups, six interviews and an overview of available evidence on peer-based, peer-led and peer-delivered needle exchange services. Peer workers from the Hepatitis C Trust and Turning Point were key members of he expert group contributing to the report.
The report found that there is strong support among people who inject drugs, peers who work with people who inject drugs, commissioners and health specialists for an innovative peer-based needle exchange service in London. A clear vision emerged from each focus group of a welcoming a service where people could access all the equipment they need (both in type and amounts), be signposted to other support where appropriate, and be treated with dignity and respect by peers who understand their circumstances.
The stigma often faced by people who inject drugs when they access high-street pharmacy services was a prominent theme in every focus group and raised in most interviews. It was felt that a peer-based service would be non-judgemental, respectful, inclusive and more attractive to people who inject drugs.
Recommendations
This report recommends, based on available international evidence and the discussions in the focus groups and interviews, that peer leadership should be embedded in the development and design of the service alongside other stakeholders in a steering committee. Peers, including both people who currently are injecting drugs and people who have previously injected drugs, should deliver the service in a range of clearly-defined roles, with training and supervision, including both paid and volunteer roles.